You don’t have to watch Tom and Jerry cartoons to know that mice run away from cats. Mice and rats are born with an innate, hardwired fear of their feline predators, and the very scent of a cat is terrifying to them. So it was quite a surprise when in 2000, parasitologist Joanne Webster found rats that had not only lost their fear of cat urine, they were attracted to it. The key feature of these rats? They were infected by the parasite Toxoplasma gondii.
This phenomenon, which Webster dubbed “fatal feline attraction,” is particularly fascinating given the peculiarities of the parasite. Toxoplasma, or Toxo for short, is seemingly able to infect just about any warm-blooded animal anywhere in the world—dogs, cows, kangaroos, koalas, chickens, pigeons, sea otters, dolphins, et al.
Yet despite its ubiquity, Toxoplasma reproduces sexually only in cats. One idea is that if Toxo-infected mice and rats become easier prey, the parasite can get into cats and complete its lifecycle. It’s a compelling story, and one made even more so by the fact that Toxo also hangs out in the brain cells of its hosts—a great location for a mind-manipulating parasite.
The more researchers have investigated how this peculiar parasitic puppetmaster can influence behavior, the more complicated the story becomes. But it’s an enigma worth figuring out, because Toxo infection has been associated with a lot of neurological problems in another species it infects—us. Toxo’s been associated with all kinds of behaviors and disorders, including schizophrenia, suicide attempts, traffic accidents, and even personality and cultural differences. (As for any theories about Toxo being the reason we like cats, or being responsible for crazy cat ladies, feel free to take those with a huge grain of salt.)
It’s still unclear how convincing some of these associations are, and figuring out how the parasite operates has taken a long and winding path with multiple dead ends. These days, researchers may finally have some promising leads about the mechanism behind Toxo’s behavioral effects. “There was a period of confusion, and kind of a wild goose chase,” said Ajai Vyas, a neurobiologist at Nanyang Technological University in Singapore. “I think that period is now gone.”
Toxo in the brain
Vyas first read about Toxoplasma’s behavioral effects in a New York Times article by Carl Zimmer. For a freshly minted PhD looking for his next research project, “it was love at first sight,” he told Ars. He decided to replicate the behavioral work with lab strains of parasites and rodents. In his experiments, Vyas typically released rats into a circular arena where opposite ends had been laced with rabbit urine or bobcat urine.
(Believe it or not, bobcat urine is commercially available and easier to get than an alternative: “With house cats, it’s very difficult to collect urine from them,” Vyas said.)
Uninfected rats avoided the bobcat urine, whereas Toxo-infected ones didn't.
Vyas found that Toxo specifically affected fear of cat odors, but not learned fear or anxiety. But if you’re imagining infected rodents throwing themselves at cats and begging to be eaten, well, Toxo’s effects are considerably subtler. “They are not fearless, they’re just a little bit less fearful,” said Vyas. “That’s exactly what you’d expect—it’s not a magic wand so that there’s no fear at all.” When Vyas used a stronger source of cat odors, such as a cat collar, the fear became overpowering and the effects disappeared. “I’m very sure if we used a real cat, we probably will not see the effect,” he said.
When trying to explain how Toxo produces this effect, Vyas initially focused on the obvious: the parasite’s presence in the brain. When Toxo infects, it barricades itself in thick-walled cysts to evade the immune system, and these cysts can remain for decades in a few sites, including the brain. If Toxo forms cysts in specific parts of the brain, it could do something there to affect behavior. But so far, different studies have found cysts in many different locations with no obvious pattern to their distribution, so it’s unclear if cyst location can influence behavior.
Another hypothesis is that Toxo affects behavior by influencing the levels of dopamine, a major neurotransmitter involved in attraction and reward behaviors. Studies suggested that Toxo infection increases dopamine levels in the brain, and it may do so by producing enzymes that are related to those involved in dopamine synthesis. This idea is particularly exciting given that increased dopamine is associated with many of the same psychological conditions—such as schizophrenia—associated with Toxo infection.
But a recent study has questioned whether Toxo infection actually increases dopamine levels, and some researchers suggest that these enzymes may not get involved in dopamine synthesis at all. Instead, some believe the enzymes provide some other function relevant to Toxo, such as building its cyst wall. So the jury’s still out on the dopamine hypothesis.
To make things even more confusing, other experiments have even questioned whether Toxo needs to form cysts in the brain in order to influence behavior.
Video of Wendy Ingram's experiments
What a difference a strain makes
Wendy Ingram was initially quite skeptical of Toxo’s ability to manipulate behavior. As a graduate student at UC Berkeley, “I actually set out to prove this whole thing wrong,” she told Ars. “Much to my surprise, it’s amazing, it’s really shocking how consistent it is that uninfected mice have an incredible aversion to cat urine, and when you infect them with Toxoplasma, there’s a loss of aversion,” said Ingram, who’s now a post-doctoral fellow at Geisinger Health System in Danville, California.
But the real breakthrough came when Ingram decided to test the effects of different strains of Toxoplasma. Toxo parasites in Europe and the US belong primarily to three distinct strains, cleverly called Type I, II and III. Most previous experiments were conducted with the Type II strain—the Type I strain was too lethal to use for behavioral experiments in mice. “You can’t study them; dead mice tell no tales,” Ingram joked.
But just in time for Ingram’s experiments, other researchers created a mutant Type I strain that, despite missing just one set of genes, displayed radically different behavior. It was now completely unable to kill mice and, unlike the Type II and Type III strains, the mutated Type I strain didn’t form cysts and hang out in the brain for the long term. Accordingly, Ingram expected it to have no effect on behavior.
To her surprise, infection with any of the three Toxo strains caused mice to lose their fear of bobcat urine. In fact, the behavior persisted even a month after infection with the type I strain, when there were no signs of Toxo cysts in their brains. The parasite appeared to have made some long-term change to behavior during its initial infection phase, which lasted just a few days. “That was kind of the most striking and most exciting thing that led us to totally rethink what everyone’s saying is true about what the mechanism could be,” said Ingram. “In the context of my results with the Type I parasite not forming cysts in the brain and getting completely cleared from the brain, from what we can tell, it has nothing to do with cysts.”
How might Toxo influence behavior without being camped out in the brain? Some intriguing new work suggests that the parasite injects its proteins into many neurons without ever forming cysts there. It’s possible that these proteins might be making some permanent changes to the neurons that influence behavior, but that’s still pretty speculative.
Nanyang Technological University’s Vyas has an alternative idea based on a completely different behavior: Toxo makes male rodents more sexually attractive.
Confusion between fear and sex
In addition to making rats less scared of cat urine, Vyas found that Toxo infection changed the way that rats interacted with each other. It made male rats more attractive to females. That’s actually quite unusual—females of many species typically avoid parasite-infected males. He also found a potential reason for Toxo to have evolved this behavioral effect: the parasite was sexually transmittable in rats. “I think it will be very difficult to come up with two separate mechanisms for these two behavioral changes, so we’re taking the view that these are both two sides of the same coin,” Vyas said.
Vyas’s current hypothesis is that the behavioral effects aren’t due to the parasite going to brain, but rather to its presence in another site where it forms cysts: the testes. Toxoplasma infection increases testosterone synthesis in male rats, and Vyas suggests that this increased testosterone mediates the production of pheromones that make males more attractive to females, as well as making changes in their brains that make them less scared of cats. “The beautiful thing about this system is that it explains both behavioral changes,” Vyas said.
Vyas’s results suggest that the Toxo-induced increase in testosterone causes epigenetic changes in a specific part of the brain that processes odor and pheromone information, which shifts the rat from wanting to hide or escape to wanting to breed. Artificially inducing similar epigenetic changes made rats less afraid of cats, even without a Toxo infection. Conversely, blocking such epigenetic changes in rats or castrating them so they couldn’t produce testosterone also blocked Toxo’s effects on the rats’ fearful response to cat urine.
Vyas also looked at neurons in this brain region (the medial amygdala) that were normally recruited by things that would make the rats want to breed, such as the presence of female rats. When male rats were infected with Toxo, these neurons were now being recruited by cat odors, a stimulus that should make them scared rather than horny. “In other words, there is a mix-up between defensive and reproductive behavior,” said Vyas. “The parasite then is just tapping into a pre-existing circuit.”
It’s an intriguing hypothesis, but it’s still preliminary and the studies need replication. Plus, there are still some loose ends to tie up—for instance, how would this mechanism work in females? Female rats show similar responses to cat urine as males when infected with Toxo, but they produce much less testosterone and have fewer of the neurons that are recruited by cat odors. Vyas is still trying to figure out whether the same testosterone-based mechanism that he posits in males would also work in females, or whether they have their own parallel circuit. Regardless, the findings do suggest a way that Toxo could cause its behavioral effects without needing to be in the brain.
Researchers are also considering the possibility that Toxo does need to be in the brain to have its effects, but the effects are indirect. “What we do know with Toxo is that it does elicit a very strong inflammatory immune response, it does get into the brain, and so the inflammatory response occurs in the brain itself, which is not a site that most microbes can get to,” said Vern Carruthers, a parasitologist at the University of Michigan. There’s an established link between immune response and behavior in the literature, an effect that’s been seen in rodents.
The idea that Toxo’s behavioral effects involve the immune system isn’t new. But Ingram’s work showed that all three Toxo strains, even the mutated one that didn’t form brain cysts, elicited a brief inflammatory response in the brain. It’s possible that this immune response makes some lasting changes to the brain, leading to a change in behavior, though a lot more work need to be done here.
If Toxo’s effects are due to the host’s immune response to it, then the parasite doesn’t have to do anything special to change the way its victims act. That raises a more basic question: does Toxo actively manipulate its host?
The parasite or the host?
We know Toxo infection causes behavioral effects. But is the parasite a devious puppetmaster, manipulating its host’s behavior to increase its transmission into cats? The behavioral manipulation hypothesis assumes that by making rodents lose their fear of cats, Toxo increases its transmission to its feline host. It’s a perfectly reasonable suggestion, but it turns out this idea is quite hard to demonstrate.
“There is no hard data either for or against the idea that behavioral changes increase transmission to cats,” said Amanda Kristancic, a zoologist at Murdoch University in Australia. Another parasite related to Toxo, Eimeria vermiformis , appears to similarly make mice less scared of cats. But unlike Toxo, this parasite doesn’t rely on cats for transmission—in fact, if cats kill the Eimeria -infected mice, the parasite would die, too. As a result, Eimeria researchers have no reason to think that the parasite causes this behavior or benefits from it, Kristancic said.
Both Nanyang Technological University’s Vyas and Geisinger Health System’s Ingram agreed that it would be important to confirm if the loss of fear caused by Toxo infection actually results in increased rodent predation. But again, that’s a hard experiment to do. “The perfect experiment would be release half mice that are infected, half mice that aren’t, in a barn that’s enclosed, and then let a couple of cats out, and catch all the mice at the end and figure out how many got eaten and which ones,” said Ingram. “But no one’s going to let you do that, it’s horrible.”
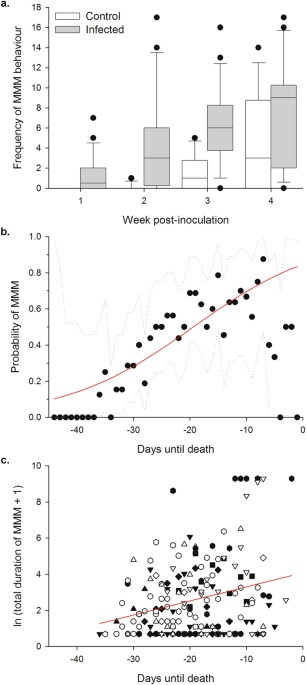
Researchers could also study Toxoplasma transmission by conducting more predation studies in the wild and in other animals. A recent study found that wild chimpanzees infected by Toxoplasma had a similar loss of aversion to the smell of leopard urine. There were only nine infected chimpanzees, and the study was correlative, so one can’t read too much into it. But it does at least open up the possibility that the loss of fear of feline predators occurs in species beyond mice and rats. Follow-up studies looking at Toxo’s effects in birds might be particularly interesting, as they’re also a prey species of cats.
What of Toxo’s effects in humans, such as its association with schizophrenia or suicide attempts? They may not require active manipulation by the parasite either. One idea is that, as in rodents, they may be the result of our body’s immune response to Toxo. For reasons that have nothing to do with this parasite, some researchers have suggested that immune and infectious causes might be responsible for a range of human behavioral effects and neurological disorders, including Alzheimer’s disease, schizophrenia, and autism. For now, it’s a hotly-debated topic. “It’s been known for a while that there are changes in the inflammatory status of the brain in people with schizophrenia,” said Carruthers. “What’s unknown is whether it’s playing a causal role or it’s just a consequence.” Similar things could be said about the other disorders.
So when it comes to humans, it turns out it can be quite hard to pin down exactly what Toxo does, let alone how it does it.
A hard thing to study
Toxoplasma infects a lot of us—almost a quarter of Americans, a third of all humans worldwide, and more than 90 percent of the population in some countries. We get it mostly from undercooked meat, or from handling cat litter or contaminated soil. Thankfully, as long as you’re healthy, it just feels just like a mild flu, although it can have more severe consequences if you’re pregnant or have a weakened immune system.
Toxo infection has also long been associated with a number of behavioral and neurological effects in humans. “ Evidence is strongest for schizophrenia, but also quite strong for affective disorders in general, and especially suicide attempts,” said Fuller Torrey, a psychiatrist at the Stanley Medical Research Institute. How does a loss of fear of cats translate to all these different effects in humans? “Very few of us are likely to be eaten by large cats, so Toxoplasma gondii doesn’t accomplish anything by getting in us, but it doesn’t know it’s in a dead-end host, it just kind of does its thing,” said Torrey. “It’s smart, but it’s not that smart.”
In interpreting the human studies, it doesn’t help that there’s still a distinct lack of scientific consensus about what effects Toxo actually has. “I still take lot of human studies with quite a bit of salt,” Nanyang Technological University’s Vyas said. “I’m not saying that the experiments are not good, but that the interpretation is fraught with a lot of complications.” Many researchers Ars spoke to pointed out that Toxo infection rates vary dramatically around the world, from a few percent of the population to more than 90 percent in some countries, whereas rates of schizophrenia are fairly constant around the world at 0.5-1 percent.
The reality is that human behavior and mental illness are complex, and many of the Toxo studies are not standardized and have yet to be replicated. Toxo certainly doesn’t make it easy to do this work—there’s no good way to detect Toxo cysts in a living person, and the studies rely on correlations with Toxo antibody levels. But antibodies are a crude measure that don’t tell you about a number of things that could affect behavior, such as when the infection occurred or which strain of the parasite you’re infected with.
To get at causation, larger studies that track people from a young age could help figure out if their behavioral symptoms show up before or after Toxo infection. Another approach would be to get rid of the parasite from an infected person who has a mental illness, and see if their clinical symptoms improve. But Toxo doesn’t let us do that yet—we currently don’t have a good way to get rid of Toxoplasma cysts once a person is infected.
The bottom-line? Toxo remains intriguing but complicated. “If there was some huge major behavioral differences, then we would have seen it by now,” said Zi Teng Wang, a parasitologist at Washington University in St. Louis. “It could be having some effect, but I wouldn’t worry about brain parasites making me crazy anytime soon.”